Student Image Challenge 100
December 5, 2023
Cardiac AL-amyloidosis [June 2023]
January 17, 2024SUBMIT YOUR CASE
EFSUMB invites submission of interesting cases for the website section 'Case of the Month'. All CoM submissions are eligible for selection for free registration at the next Euroson congress. Two cases that receive the most 'likes' in a year will receive free registration for the next EUROSON congress and the third most liked liked case will receive a cash prize of 100 EUR.
Detection of a micrometastasis using elastography - a promising method
Authors: Rink M[1], Krassler J[1], Symeou L[1], Jung EM[2], Bohr C[1], Künzel J[1]
[1] Department of Otorhinolaryngology, University Hospital Regensburg, 93053 Regensburg, Germany[2] Department of Radiology, University Hospital Regensburg, 93053 Regensburg, Germany
1Clinical History
The 49-year-old patient consulted us because of a tongue ulcer that had been present for approximately 3 months. This ulcer had progressed in size over the last few weeks. Eating and drinking were still possible. There was a positive history for nicotine and alcohol. Clinical suspicion of carcinoma at the lateral aspect of the tongue led to hospitalization for panendoscopy.
2Image findings
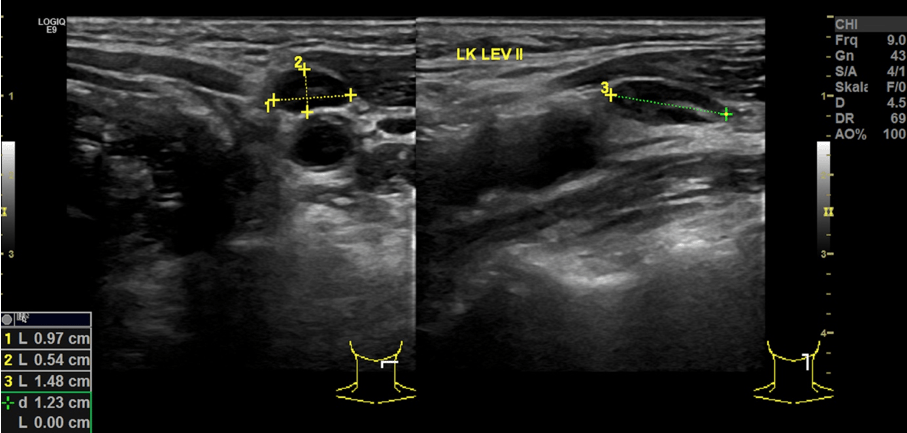
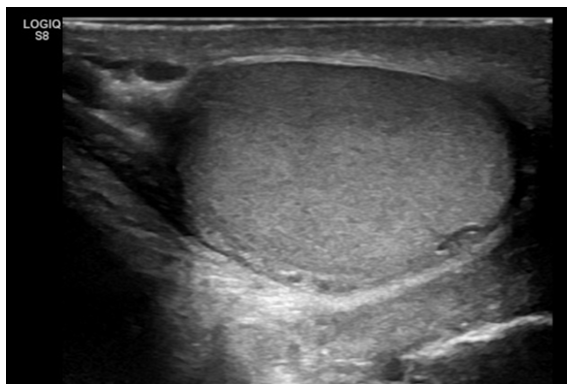
In addition to confirming the diagnosis via panendoscopy, staging was performed using contrast enhanced CT of the neck and thorax, as well as sonography of the abdomen. There were no signs of distant metastasis. In the cross sectional imaging, cervical lymph nodes were found to be unremarkable overall, but a follow-up was recommended for a node in the level IIb due to a diameter of 9 mm. In addition, sonography of the neck was performed. Conventional sonography revealed a cN0 status, and the lymph node described in the CT scan did not appear suspicious on the B-scan (see Figure 1). The suspected tumor was classified as cT1cN0cM0 (UICC Stage II) at this point.
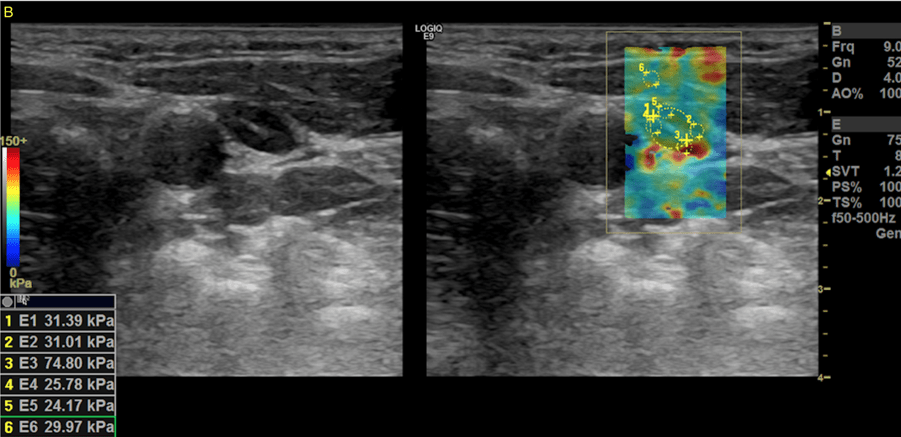
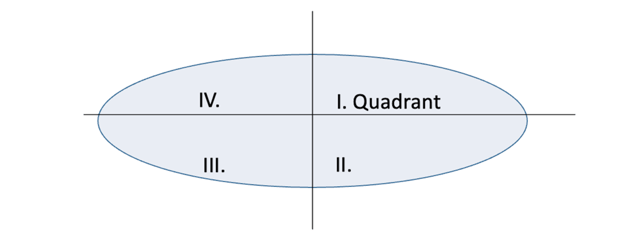
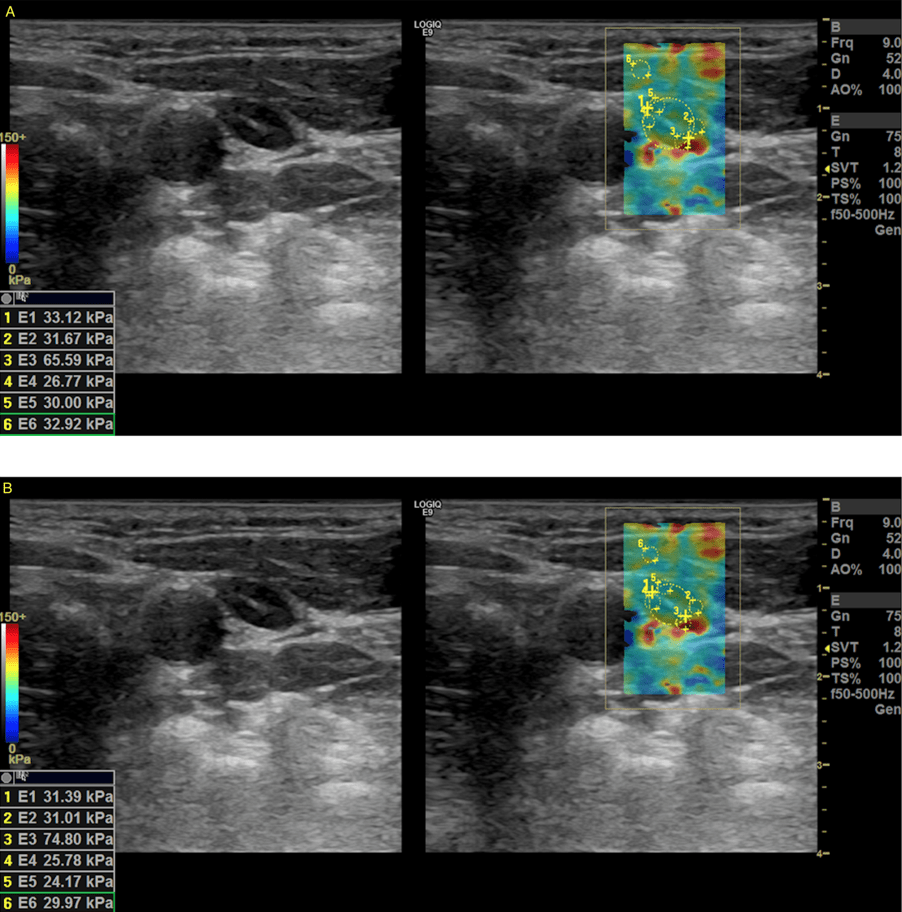
As part of a prospective study on the use of elastography in the primary staging of head and neck cancer patients, the lymph nodes that could be visualized sonographically in the patient were also examined using shear wave elastography. The measurements were taken in four quadrants (see Figure 2). Increased stiffness values were repeatedly found for the node described, particularly in the second quadrant (see Figure 3).
As part of a prospective study on the use of elastography in the primary staging of head and neck cancer patients, the lymph nodes that could be visualized sonographically in the patient were also examined using shear wave elastography. The measurements were taken in four quadrants (see Figure 2). Increased stiffness values were repeatedly found for the node described, particularly in the second quadrant (see Figure 3).
3Diagnosis
Carcinoma of the left tongue (pT2pN2bcM0, UICC Stage IVA) with lymph node metastases in two of ten removed lymph nodes.
4Discussion
BACKGROUND:
Head and neck squamous cell carcinoma (HNSCC) is one of the most common tumor entities worldwide, with frequent lymphatic metastasis in advanced stages (1,2). Regardless of the chosen method, 20-30% of lymph node metastases are not detected during primary staging (3,4). As a result, elective neck dissection is often performed even in a cN0 stage (5,6). Thus, there is a need for improved imaging to determine the best individual therapy for a patient.
Shear wave elastography offers a possible approach for this. An acoustic signal is used to generate shear waves, the propagation speed of which is then measured and displayed graphically. In addition, "regions of interest" can be defined for which the propagation speed is then measured (7). Recent studies show promising results in using elastography to achieve improved differentiation between benign and malignant nodes, particularly in small cervical lymph nodes (8,9). However, established, non device- and manufacturer-dependent reference values are still lacking.
CLINICAL PERSPECTIVE:
Symptoms of HNSCC depend to a large extent on the exact location and size of the tumor. Typical symptoms include pain, particularly when eating, difficulty swallowing, a deterioration in the general condition and, in the case of tumors located further caudal, changes in the voice or shortness of breath.
THERAPY PLANNING:
The treatment of HNSCC should always be determined by an interdisciplinary tumor board. Depending on the location, size, staging results and patient-specific factors, a decision is usually made between surgery and primary radiochemotherapy. In some cases, both forms of therapy can be presented to the patient as equal alternatives. In the present case, the tumor board recommended surgical treatment.
OUTCOME & PROGNOSIS:
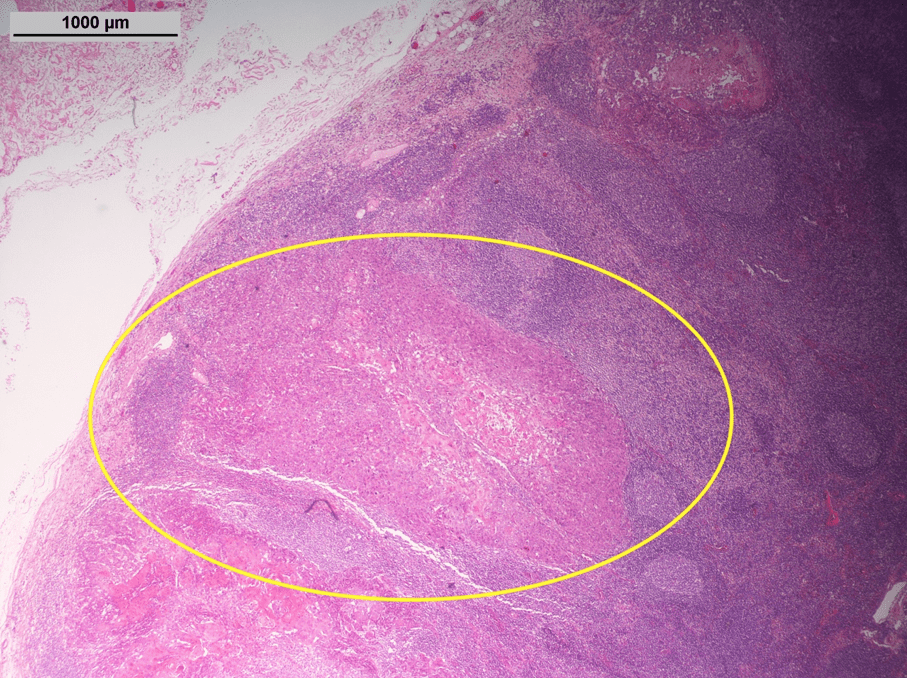
The patient underwent resection of the tumor and unilateral neck dissection of the left side. A metastasis of squamous cell carcinoma was confirmed in the elastographically suspicious lymph node (see Figure 4). Histopathology revealed a pT2pN2b status. Therefore, there was an indication for additional neck dissection of the opposite side, which was performed as a second operation in the later course. Following the tumor board decision, adjuvant radiotherapy was also performed.
Prognosis in HNSCC is highly dependent on localization, size of the primary tumor and many other factors. The presence of lymph node metastases, especially multiple ones, significantly worsens the prognosis (10).
Head and neck squamous cell carcinoma (HNSCC) is one of the most common tumor entities worldwide, with frequent lymphatic metastasis in advanced stages (1,2). Regardless of the chosen method, 20-30% of lymph node metastases are not detected during primary staging (3,4). As a result, elective neck dissection is often performed even in a cN0 stage (5,6). Thus, there is a need for improved imaging to determine the best individual therapy for a patient.
Shear wave elastography offers a possible approach for this. An acoustic signal is used to generate shear waves, the propagation speed of which is then measured and displayed graphically. In addition, "regions of interest" can be defined for which the propagation speed is then measured (7). Recent studies show promising results in using elastography to achieve improved differentiation between benign and malignant nodes, particularly in small cervical lymph nodes (8,9). However, established, non device- and manufacturer-dependent reference values are still lacking.
CLINICAL PERSPECTIVE:
Symptoms of HNSCC depend to a large extent on the exact location and size of the tumor. Typical symptoms include pain, particularly when eating, difficulty swallowing, a deterioration in the general condition and, in the case of tumors located further caudal, changes in the voice or shortness of breath.
THERAPY PLANNING:
The treatment of HNSCC should always be determined by an interdisciplinary tumor board. Depending on the location, size, staging results and patient-specific factors, a decision is usually made between surgery and primary radiochemotherapy. In some cases, both forms of therapy can be presented to the patient as equal alternatives. In the present case, the tumor board recommended surgical treatment.
OUTCOME & PROGNOSIS:
The patient underwent resection of the tumor and unilateral neck dissection of the left side. A metastasis of squamous cell carcinoma was confirmed in the elastographically suspicious lymph node (see Figure 4). Histopathology revealed a pT2pN2b status. Therefore, there was an indication for additional neck dissection of the opposite side, which was performed as a second operation in the later course. Following the tumor board decision, adjuvant radiotherapy was also performed.
Prognosis in HNSCC is highly dependent on localization, size of the primary tumor and many other factors. The presence of lymph node metastases, especially multiple ones, significantly worsens the prognosis (10).
5Teaching Points
Ultrasound of the neck plays a decisive role in staging HNSCC to determine the correct therapy. Shear wave elastography offers great potential to improve the detection of metastases. In the present case, B-scan criteria were not suspicious. Only shear wave elastography showed signs of malignancy. Further studies are required for standardization.
6References
1.) Ferlay J, Colombet M, Soerjomataram I, et al. Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. Int J Cancer 2019; 144(8): 1941–53.
2.) Chen LY, Weng WB, Wang W, Chen JF. Analyses of high-risk factors for cervical lymph node metastasis in laryngeal squamous cell carcinoma and establishment of nomogram prediction model. Ear Nose Throat J 2021; 100(5_suppl): 657S-662S.
3.) Garrel R, Poissonnet G, Moyà Plana A, et al. Equivalence randomized trial to compare treatment on the basis of sentinel node biopsy versus neck node dissection in operable T1-T2N0 oral and oropharyngeal cancer. J Clin Oncol. 2020; 38(34): 4010–4018.
4.) Hasegawa Y, Tsukahara K, Yoshimoto S, et al. Neck dissections based on sentinel lymph node navigation versus elective neck dissections in early oral cancers: a randomized, multicenter, and noninferiority trial. J Clin Oncol. 2021; 39(18): 2025-2036
5.) Paleri V, Urbano TG, Mehanna H, et al. Management of neck metastases in head and neck cancer: United Kingdom National Multidisciplinary Guidelines. J Laryngol Otol. 2016; 130(S2): S161–S169.
6.) D’Cruz AK, Vaish R, Kapre N, et al. Elective versus therapeutic neck dissection in node-negative oral cancer. N Engl J Med. 2015; 373(6): 521–529.
7.) Sigrist RMS, Liau J, Kaffas AE, Chammas MC, Willmann JK. Ultrasound elastography: review of techniques and clinical applications. Theranostics. 2017; 7(5): 1303–1329.
8.) Lerchbaumer MH, Wakonig KM, Arens P, Dommerich S, Fischer T. Quantitative multiparametric ultrasound (mpUS) in the assessment of inconclusive cervical lymph nodes. Cancers. 2022; 14(7): 1597.
9.) Künzel J, Brandenstein M, Zeman F, Symeou L, Platz Batista da Silva N, Jung EM. Multiparametric ultrasound of cervical lymph node metastases in head and neck cancer for planning non-surgical therapy. Diagnostics. 2022; 12(8): 1842.
10.) Arun I, Maity N, Hameed S, et al. Lymph node characteristics and their prognostic significance in oral squamous cell carcinoma. Head & Neck. 2021; 43(2): 520–533.
2.) Chen LY, Weng WB, Wang W, Chen JF. Analyses of high-risk factors for cervical lymph node metastasis in laryngeal squamous cell carcinoma and establishment of nomogram prediction model. Ear Nose Throat J 2021; 100(5_suppl): 657S-662S.
3.) Garrel R, Poissonnet G, Moyà Plana A, et al. Equivalence randomized trial to compare treatment on the basis of sentinel node biopsy versus neck node dissection in operable T1-T2N0 oral and oropharyngeal cancer. J Clin Oncol. 2020; 38(34): 4010–4018.
4.) Hasegawa Y, Tsukahara K, Yoshimoto S, et al. Neck dissections based on sentinel lymph node navigation versus elective neck dissections in early oral cancers: a randomized, multicenter, and noninferiority trial. J Clin Oncol. 2021; 39(18): 2025-2036
5.) Paleri V, Urbano TG, Mehanna H, et al. Management of neck metastases in head and neck cancer: United Kingdom National Multidisciplinary Guidelines. J Laryngol Otol. 2016; 130(S2): S161–S169.
6.) D’Cruz AK, Vaish R, Kapre N, et al. Elective versus therapeutic neck dissection in node-negative oral cancer. N Engl J Med. 2015; 373(6): 521–529.
7.) Sigrist RMS, Liau J, Kaffas AE, Chammas MC, Willmann JK. Ultrasound elastography: review of techniques and clinical applications. Theranostics. 2017; 7(5): 1303–1329.
8.) Lerchbaumer MH, Wakonig KM, Arens P, Dommerich S, Fischer T. Quantitative multiparametric ultrasound (mpUS) in the assessment of inconclusive cervical lymph nodes. Cancers. 2022; 14(7): 1597.
9.) Künzel J, Brandenstein M, Zeman F, Symeou L, Platz Batista da Silva N, Jung EM. Multiparametric ultrasound of cervical lymph node metastases in head and neck cancer for planning non-surgical therapy. Diagnostics. 2022; 12(8): 1842.
10.) Arun I, Maity N, Hameed S, et al. Lymph node characteristics and their prognostic significance in oral squamous cell carcinoma. Head & Neck. 2021; 43(2): 520–533.